- I encourage facilities to have a written and formal fall program. This program should take a continuous quality improvement approach to falls. There are many ways to accomplish this, and I have provided some resources below. There are some interventions that probably should be implemented when a resident falls more than once and no root cause has been identified.
- Post fall huddle (ASAP!)
- ASAP, with the CNAs and nurses that identified the fall
- Root cause analysis
- Environment evaluation
- Accidental fall?
- Spill on floor, trip on oxygen tubing, slipped in transition, etc…
- Interventions planned
- Review interventions daily for 30 days to assess success of intervention
- Document intervention and efficacy of intervention.
- Change in condition?
- New onset medical condition
- Postural hypotension
- Dizziness
- confusion
- new medication
- progression of dementia or other chronic disease state
- Accidental fall?
- Vital signs.
- Orthostatic blood pressure and heart rate
- Check glucose
- Alert physician
- Collect the information above within 24 hours.
- Once you have the above information collected, present the case to the patient’s attending physician.
- PT evaluation
- Vision assessment – PT can do a functional visual assessment
- Physician evaluation for falls
- Physical exam and labs/imaging aimed at identifying causes of falling, weakness, dizziness, functional decline, or other potential change in medical status that could increase fall risk.
- Physician note outlining recognition of falls, plan for workup, potential causes, interventions, lab/imaging results, and expectation for successful interventions.
Intervention List:
https://docs.google.com/spreadsheets/d/1UT32dAtnjoRRUtSytngcUWavwg0ZarkliIXEeMVY7m0/edit?usp=sharing
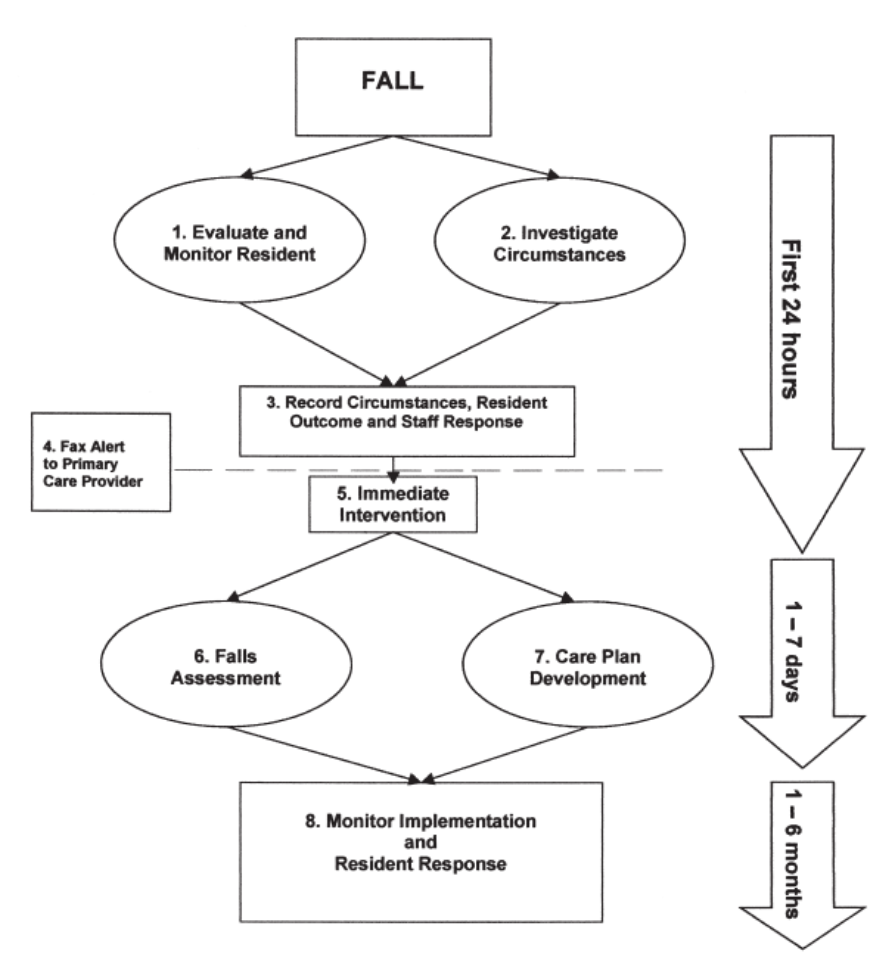
Fall Evaluation Tools – docShepherd
Falls and Vision Impairment – docShepherd
